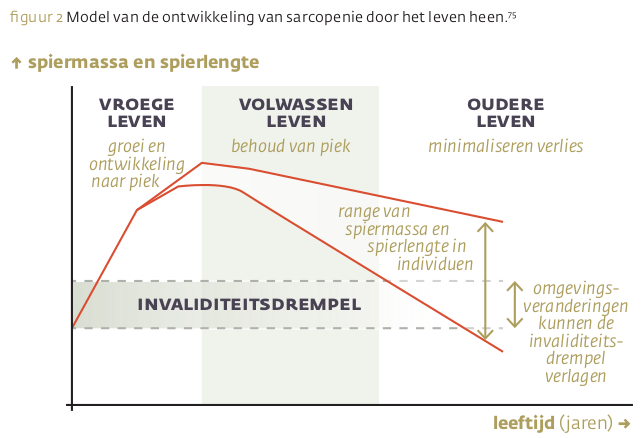
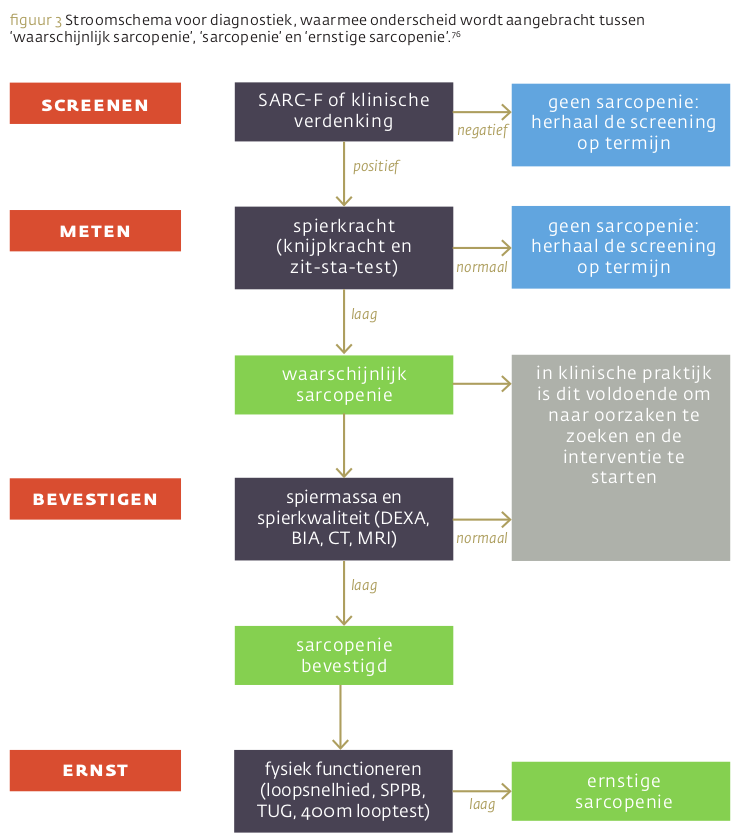
Veroudering brengt een verscheidenheid aan veranderingen in het lichaam met zich mee. Een hiervan kan leeftijdsgebonden sarcopenie zijn. Dit verlies aan spiermassa en -kracht houdt verband met fysieke en cognitieve beperkingen, verminderde kwaliteit van leven en een verhoogde kans op overlijden. Voor preventie en behandeling zijn, naast onder meer hormoonbehandeling, diverse leefstijlinterventies beschikbaar.
Beste bezoeker, u heeft geen toegang.
Enkel (web)abonnees hebben toegang tot tijdschriftartikelen. Het webabonnement is nog in de maak.
U kunt zich wel alvast (gratis) registreren en tal van andere webartikelen raadplegen!
Auteur
Trefwoorden:
Verschenen in
Referenties
- Rosenberg IH. Summary comments: epidemiological and methodological problems in determining nutritional status of older persons. Am J Clin Nutr. 1989;50:1231-3
Giesbers H, Verweij A, Beer J. de. Vergrijzing: Wat zijn de belangrijkste verwachtingen voor de toekomst? In: Volksgezondheid Toekomstverkenning, Nationaal Kompas Volksgezondheid, RIVM, Bilthoven, 26 september 2013.
Flatt T. A new definition of aging? Front Genet. 2012;3:148
Curcio F, Ferro G, Basile C, et al. Biomarkers in sarcopenia: a multifactorial approach. Exp Gerontol. 2016;85:1–8.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM et al. Sarcopenia: European consensus on definition and diagnosis. Report of the European Working Group on Sarcopenia in Older People. J. Cruz-Gentoft et al. Age and ageing, 2010, 39.4: 412-423.
Cao L., Morley JE, Sarcopenia is recognized as an independent condition by an international classification of disease, tenth revision, clinical modification (ICD-10-CM) code. Journal of the American Medical Directors Association, 2016, 17.8: 675-677.
Bijlsma, A. Y., et al. Defining sarcopenia: the impact of different diagnostic criteria on the prevalence of sarcopenia in a large middle aged cohort. Age, 2013, 35.3: 871-881.
Beenakker, KGM, et al. Patterns of muscle strength loss with age in the general population and patients with a chronic inflammatory state. Ageing research reviews, 2010, 9.4: 431-436.
Buford, T.W., et al. Models of accelerated sarcopenia: critical pieces for solving the puzzle of age-related muscle atrophy. Ageing research reviews, 2010, 9.4: 369-383.
Cruz-Jentoft AJ., et al. Prevalence of and interventions for sarcopenia in ageing adults: a systematic review. Report of the International Sarcopenia Initiative (EWGSOP and IWGS). Age and ageing, 2014, 43.6: 748-759.
Janssen, I., et al. Skeletal muscle cutpoints associated with elevated physical disability risk in older men and women. American journal of epidemiology, 2004, 159.4: 413-421.
Bunout, D., et al. Association between sarcopenia and mortality in healthy older people. Australasian journal on ageing, 2011, 30.2: 89-92.
Sternberg, S. A., et al. The identification of frailty: a systematic literature review. Journal of the American Geriatrics Society, 2011, 59.11: 2129-2138.
Janssen, I., et al.. The healthcare costs of sarcopenia in the United States. Journal of the American Geriatrics Society, 2004, 52.1: 80-85.
Beaudart, C., et al. Health outcomes of sarcopenia: a systematic review and meta-analysis. PloS one, 2017, 12.1: e0169548.
Abete, P., et al. The Italian version of the “frailty index” based on deficits in health: a validation study. Aging clinical and experimental research, 2017, 29.5: 913-926.
Rochefort, G. Y., Pallu, S.; Benhamou, CL. Osteocyte: the unrecognized side of bone tissue. Osteoporosis international, 2010, 21.9: 1457-1469.
Jager-Wittenaar,H. Wat is sarcopenie NED TIJDSCHR VOOR VOEDING & DIËTETIEK - 2018;73(T): 35
Calvani, R., et al. Biomarkers for physical frailty and sarcopenia. Aging clinical and experimental research, 2017, 29.1: 29-34.
Shaw, S. C.; Dennisson, E. M.; Cooper, C. Epidemiology of sarcopenia: determinants throughout the lifecourse. Calcified tissue international, 2017, 101.3: 229-247.
Woo, J.. Sarcopenia. Clinics in geriatric medicine, 2017, 33.3: 305-314.
Landi, F., et al. Anorexia of aging: risk factors, consequences, and potential treatments. Nutrients, 2016, 8.2: 69.
Schilp J., et al. Effect diëtist bij ondervoede thuiswonende ouderen. Huisarts & wetenschap, 56(10) oktober 2013: 498-501
Ali, S., Garcia, J. M. Sarcopenia, cachexia and aging: diagnosis, mechanisms and therapeutic options-a mini-review. Gerontology, 2014, 60.4: 294-305.
Fiatarone, M. A., et al. High-intensity strength training in nonagenarians: effects on skeletal muscle. Jama, 1990, 263.22: 3029-3034.
Fiatarone, M. A., et al. Exercise training and nutritional supplementation for physical frailty in very elderly people. New England Journal of Medicine, 1994, 330.25: 1769-1775.
Hurley, B., Roth, S. M. Strength training in the elderly. Sports medicine, 2000, 30.4: 249-268.
Burton, L. A.; Sumukadas, D. Optimal management of sarcopenia. Clinical interventions in aging, 2010, 5: 217.
Calvani, R., et al. Current nutritional recommendations and novel dietary strategies to manage sarcopenia. The Journal of frailty & aging, 2013, 2.1: 38.
Robinson, S. M., et al. Diet and its relationship with grip strength in community‐dwelling older men and women: The Hertfordshire Cohort Study. Journal of the American Geriatrics Society, 2008, 56.1: 84-90.
Shahar, D. R., et al. Adherence to Mediterranean diet and decline in walking speed over 8 years in community‐dwelling older adults. Journal of the American Geriatrics Society, 2012, 60.10: 1881-1888.
Leon-Munoz, L. M., et al. Mediterranean diet and risk of frailty in community-dwelling older adults. Journal of the American Medical Directors Association, 2014, 15.12: 899-903.
Zbeida, M., et al. Mediterranean diet and functional indicators among older adults in non-Mediterranean and Mediterranean countries. The journal of nutrition, health & aging, 2014, 18.4: 411-418.
Bollwein, J., et al. Dietary quality is related to frailty in community-dwelling older adults. Journals of Gerontology Series A: Biomedical Sciences and Medical Sciences, 2012, 68.4: 483-489.
Morley, J. E., et al. Nutritional recommendations for the management of sarcopenia. Journal of the american Medical Directors association, 2010, 11.6: 391-396.
Gaffney‐Stomberg, E., et al. Increasing dietary protein requirements in elderly people for optimal muscle and bone health. Journal of the American Geriatrics Society, 2009, 57.6: 1073-1079.
ArnalL, M.A., et al. Protein pulse feeding improves protein retention in elderly women. The American journal of clinical nutrition, 1999, 69.6: 1202-1208.
Morley, J. E., et al. Pharmacologic options for the treatment of sarcopenia. Calcified tissue international, 2016, 98.4: 319-333.
Bauer, J., et al. Evidence-based recommendations for optimal dietary protein intake in older people: a position paper from the PROT-AGE Study Group. Journal of the american Medical Directors association, 2013, 14.8: 542-559.
Volpi, E., et al. Is the optimal level of protein intake for older adults greater than the recommended dietary allowance?. Journals of Gerontology Series A: Biomedical Sciences and Medical Sciences, 2012, 68.6: 677-681.
Gezondheidsraad. Ondervoeding bij ouderen, nr. 2011/32. Den Haag, 2011
Boirie, Y. Physiopathological mechanism of sarcopenia. JNHA-The Journal of Nutrition, Health and Aging, 2009, 13.8: 717-723.
Paddon-Jones, D., Rasmussen, B. B. Dietary protein recommendations and the prevention of sarcopenia: Protein, amino acid metabolism and therapy. Current opinion in clinical nutrition and metabolic care, 2009, 12.1: 86.
Symons, T. B., et al. A moderate serving of high-quality protein maximally stimulates skeletal muscle protein synthesis in young and elderly subjects. Journal of the American Dietetic Association, 2009, 109.9: 1582-1586.
Wilson, G. J.; Wilson, J. M.; Manninen, A. H. Effects on beta-hydroxy-betamethylbutyrate (HMB) on exercise levels of age, sex and training experience: A review. Nutrition & Metabolism, 2008, 5.1: 1-10.1186.
Houston, D. K., et al. Dietary protein intake is associated with lean mass change in older, community-dwelling adults: the Health, Aging, and Body Composition (Health ABC) Study. The American journal of clinical nutrition, 2008, 87.1: 150-155.
Tieland, M., et al. Protein supplementation increases muscle mass gain during prolonged resistance-type exercise training in frail elderly people: a randomized, double-blind, placebo-controlled trial. Journal of the American Medical Directors Association, 2012, 13.8: 713-719.
Leenders, Marika; van Loon, L.J.C. Leucine as a pharmaconutrient to prevent and treat sarcopenia and type 2 diabetes. Nutrition reviews, 2011, 69.11: 675-689.
DEUTZ, Nicolaas EP, et al. Protein intake and exercise for optimal muscle function with aging: recommendations from the ESPEN Expert Group. Clinical nutrition, 2014, 33.6: 929-936.
Volpi, E., et al. Essential amino acids are primarily responsible for the amino acid stimulation of muscle protein anabolism in healthy elderly adults. The American journal of clinical nutrition, 2003, 78.2: 250-258.
Layman, D.K., et al. Defining meal requirements for protein to optimize metabolic roles of amino acids. The American journal of clinical nutrition, 2015, 101.6: 1330S-1338S.
Devries, M. C., et al. Leucine, not total protein, content of a supplement is the primary determinant of muscle protein anabolic responses in healthy older women. The Journal of nutrition, 2018, 148.7: 1088-1095.
Devries, M. C., et al.., et al. Protein leucine content is a determinant of shorter-and longer-term muscle protein synthetic responses at rest and following resistance exercise in healthy older women: a randomized, controlled trial. The American journal of clinical nutrition, 2018, 107.2: 217-226.
Eliot, K. A., et al. The effects of creatine and whey protein supplementation on body composition in men aged 48 to 72 years during resistance training. The Journal of Nutrition Health and Aging, 2008, 12.3: 208.
Cermak, N. M., et al. Protein supplementation augments the adaptive response of skeletal muscle to resistance-type exercise training: a meta-analysis. The American journal of clinical nutrition, 2012, 96.6: 1454-1464.
Van Dongen, E. JI, et al. Effect, process, and economic evaluation of a combined resistance exercise and diet intervention (ProMuscle in Practice) for community-dwelling older adults: design and methods of a randomised controlled trial. BMC public health, 2018, 18.1: 877.
Van Schoor, N.; Lips, P. Worldwide vitamin D status. In: Vitamin D. Academic Press, 2018. p. 15-40.
Annweiler, C., et al. Vitamin D-related changes in physical performance: a systematic review. The journal of nutrition, health & aging, 2009, 13.10: 893-898.
Muir, S. W. et al. Effect of vitamin D supplementation on muscle strength, gait and balance in older adults: a systematic review and meta‐analysis. Journal of the American Geriatrics Society, 2011, 59.12: 2291-2300. J. Am. Geriatr. Soc. 2011, 59, 2291–2300.
Rosendahl‐Riise, H. et al. Vitamin D supplementation and its influence on muscle strength and mobility in community‐dwelling older persons: a systematic review and meta‐analysis. Journal of human nutrition and dietetics, 2017, 30.1: 3-15.
Beaudart, C., et al. The effects of vitamin D on skeletal muscle strength, muscle mass, and muscle power: a systematic review and meta-analysis of randomized controlled trials. The Journal of Clinical Endocrinology & Metabolism, 2014, 99.11: 4336-4345.
Lauretani, F., et al. Carotenoids as protection against disability in older persons. Rejuvenation research, 2008, 11.3: 557-563.
Lauretani, F., et al. Low plasma carotenoids and skeletal muscle strength decline over 6 years. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences, 2008, 63.4: 376-383.
Bjelakovic, G., et al. Mortality in randomized trials of antioxidant supplements for primary and secondary prevention: systematic review and meta-analysis. Jama, 2007, 297.8: 842-857.
Ewaschuk, J. B., et al.Role of n-3 fatty acids in muscle loss and myosteatosis. Applied Physiology, Nutrition, and Metabolism, 2014, 39.6: 654-662.
Gray, S.R.,Mittendorfer, B.. Fish oil-derived n-3 polyunsaturated fatty acids for the prevention and treatment of sarcopenia. Current Opinion in Clinical Nutrition & Metabolic Care, 2018, 21.2: 104-109.
Lalia, A.Z., et al. Influence of omega-3 fatty acids on skeletal muscle protein metabolism and mitochondrial bioenergetics in older adults. Aging (Albany NY), 2017, 9.4: 1096.
Hutchins-Wiese, H. L. et al. The impact of supplemental n-3 long chain polyunsaturated fatty acids and dietary antioxidants on physical performance in postmenopausal women. The journal of nutrition, health & aging, 2013, 17.1: 76-80.
Smith. G. I., et al. Fish oil–derived n− 3 PUFA therapy increases muscle mass and function in healthy older adults. The American journal of clinical nutrition, 2015, 102.1: 115-122.
Logan, S. L.; Spriet, L. L. Omega-3 fatty acid supplementation for 12 weeks increases resting and exercise metabolic rate in healthy community-dwelling older females. PLoS One, 2015, 10.12: e0144828.
Ticinesi, A., et al. Aging gut microbiota at the cross-road between nutrition, physical frailty, and sarcopenia: is there a gut–muscle axis?. Nutrients, 2017, 9.12: 1303.
Buigues, Cristina, et al. Effect of a prebiotic formulation on frailty syndrome: a randomized, double-blind clinical trial. International journal of molecular sciences, 2016, 17.6: 932.
Bell, K. E., et al. A whey protein-based multi-ingredient nutritional supplement stimulates gains in lean body mass and strength in healthy older men: A randomized controlled trial. PLoS One, 2017, 12.7: e0181387.
Bo, Y., et al.. A high whey protein, vitamin D and E supplement preserves muscle mass, strength, and quality of life in sarcopenic older adults: A double-blind randomized controlled trial. Clinical Nutrition, 2019, 38.1: 159-164.
Sayer, A. A., et al. The developmental origins of sarcopenia. The Journal of Nutrition Health and Aging, 2008, 12.7: 427.
Cruz-Jentoft A, Bahat G, Bauer J, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 2018 Oct 12.
Kruizenga H. NED TIJDSCHR VOOR VOEDING & DIËTETIEK - 2018;73(6):15
Diet of community-dwelling older adults. Dutch National Food Consumption Survey-Older adults 2010-2012.